Intelligent networks made easy
We believe provider networks should be your biggest asset—not your biggest obstacle.

J2 helps health plans manage network adequacy, optimize provider networks, and move faster with clear, actionable intelligence.
Trusted by 30+ healthcare organizations nationwide
















Replace fragmented legacy tools with a faster, clearer way to manage provider networks.
Simplify network adequacy compliance and reporting
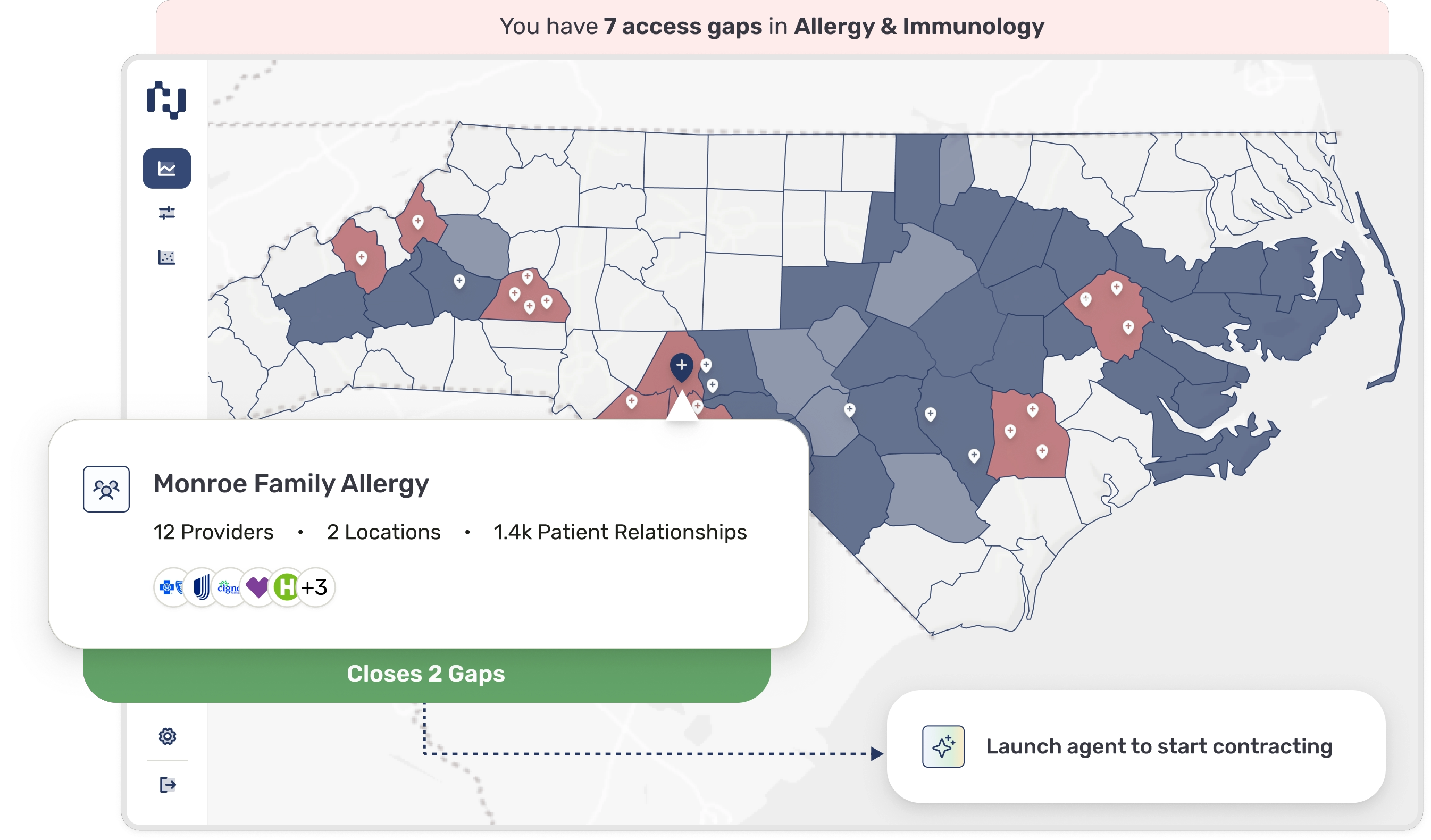
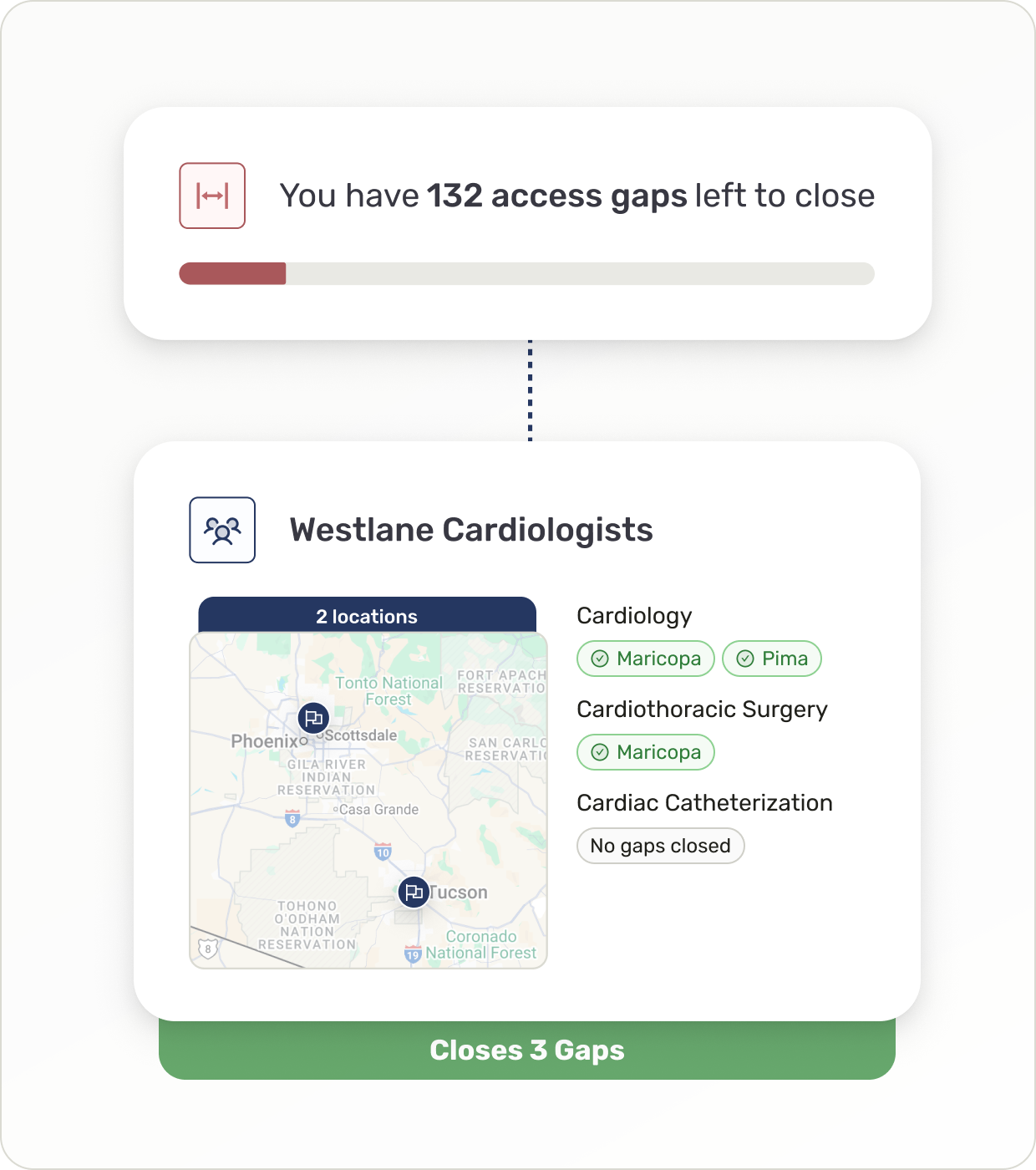
Identify and close provider network gaps in minutes, not weeks
Measure network adequacy using trusted provider data and market intelligence
Manage CMS, state, and employer network adequacy requirements in one platform
Build competitive provider networks that attract and retain members
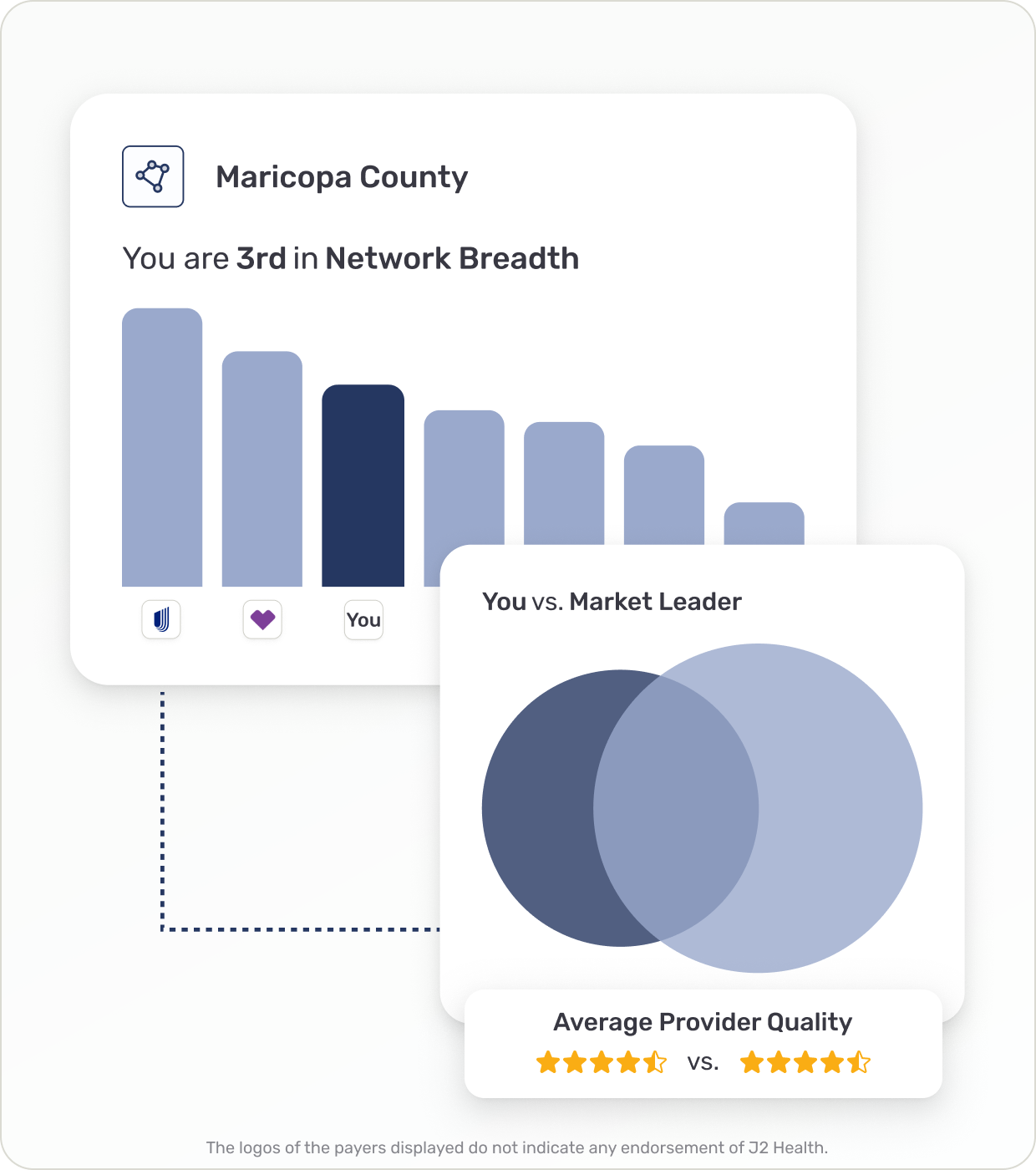
Benchmark your network against competitors in your market
Identify providers that influence enrollment, retention, and member access
Design tailored provider networks based on performance, access, and strategic goals
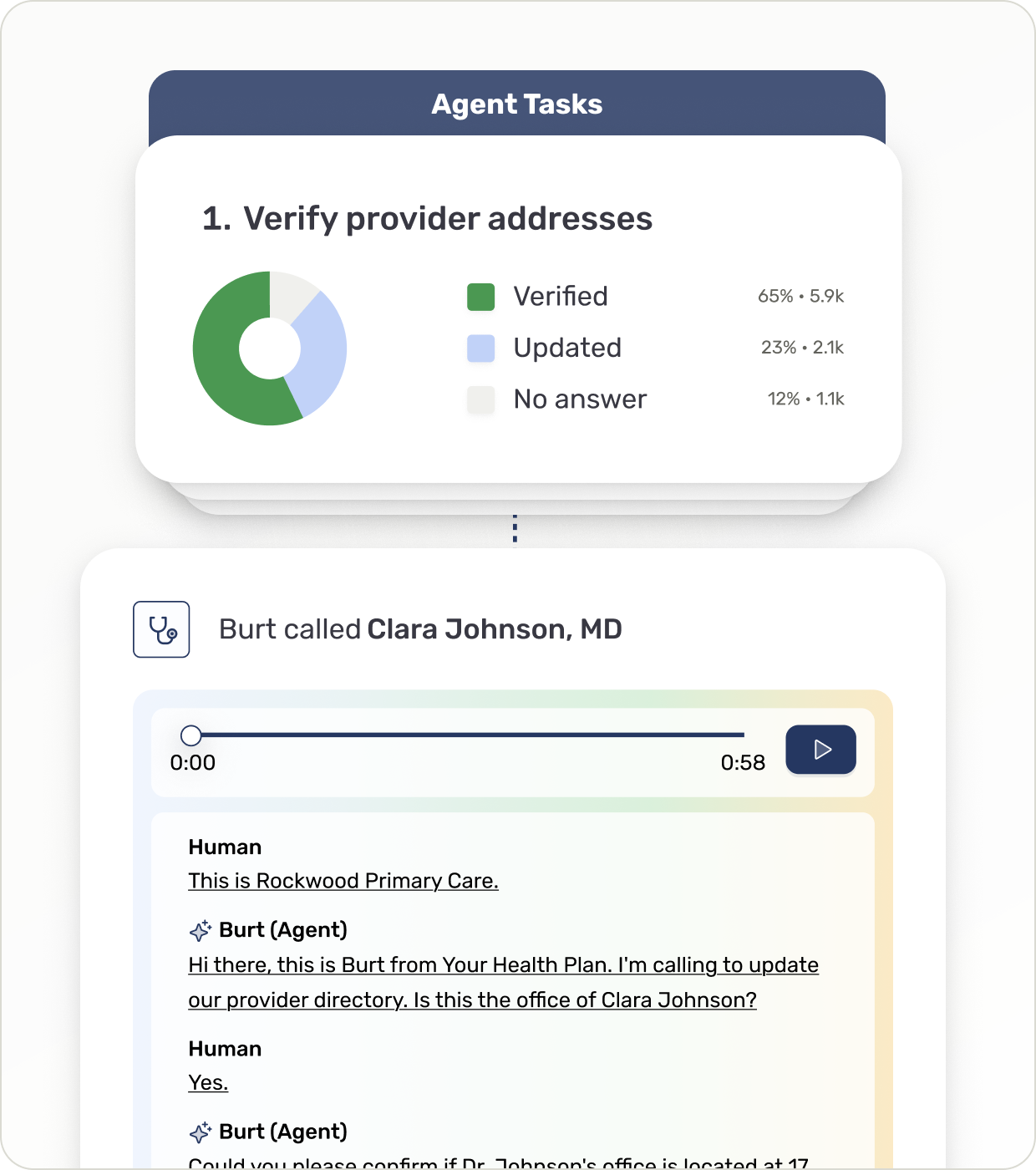
Automate provider outreach and data collection
Collect provider demographics directly from providers
Confirm network participation and appointment availability
Conduct CMS, state, and NCQA regulatory outreach with less manual effort
Why we’re different
Built by people who’ve managed provider networks themselves
Trusted provider data designed for real-world network decisions
Faster workflows that reduce manual effort and complexity
A high-touch partner approach—not just another vendor

A trusted partner
A trusted partner

for your network goals
for your network goals
A trusted partner

A trusted partner
A trusted partner

for your network goals
for your network goals
A trusted partner

A trusted partner
A trusted partner

for your network goals
for your network goals
A trusted partner

A trusted partner
A trusted partner

for your network goals
for your network goals
A trusted partner

Our impact
30+
Trusted health plans nationwide
20%
YoY customer growth
25%
Average cost savings for customers
